The Link Between Antiphospholipid Syndrome and Pregnancy Outcomes: What You Need to Know

Severe Pollution, AQI Levels Highly Dangerous For Pregnant Women, Fetus; Expert-backed Ways To Protect Yourself The Link Between Antiphospholipid Syndrome and Pregnancy Outcomes: What You Need to Know Source: The Hindu – Health Antiphospholipid Syndrome (APS) is a medical condition that often does not appear easily at the surface of clinical situations, even though it may be present. It does not have the instant recognisability of diabetes, hypertension, or thyroid disorders, yet its impact can be life-changing, particularly for women in their reproductive years. Understanding APS APS is an autoimmune disorder in which the body mistakenly produces antibodies that attack phospholipids, a type of fat essential for normal blood vessel function. This deviation leads to an increased tendency of blood clot formation in both veins and arteries. If unnoticed or not treated, APS can cause complications ranging from deep vein thrombosis to recurrent miscarriages. Although considered rare, APS is not as uncommon as perceived. Studies suggest that APS affects 1–5% of the general population, and up to 10–15% of women with recurrent pregnancy loss test positive for antiphospholipid antibodies. Many individuals live with APS silently until a major event such as a stroke, clot, or miscarriage reveals it. Impacts on Pregnancy One of the most critical reasons to tackle APS is its strong link with pregnancy complications. APS is one of the leading treatable causes of recurrent miscarriages, especially after 10 weeks of gestation. It can also cause: Recurrent early pregnancy loss Gestational hypertension or eclampsia Severe foetal growth restriction Preterm delivery due to placental insufficiency Without awareness, these complications may be taken as “bad luck” or “natural losses.” Timely diagnosis, however, can dramatically improve chances of continuation of pregnancy and healthy outcomes. With proper treatment, which usually consists of low dose aspirin and heparin injections, live birth rates can rise significantly. Misconceptions and Mimicking Conditions A common misconception is that clotting disorders only affect the elderly or those with heart disease. APS defies this belief. Many patients are young, in their 20s or 30s, with none of the traditional risk factors. APS can also often mimic other conditions. Because symptoms vary widely—headaches, skin changes, repeated miscarriages, unexplained clots and low platelet count—APS can be confused with other conditions including lupus, thrombophilia, or simple vascular disorders. How Is It Treated? APS is not curable, but it is manageable. Treatment aims to reduce clot risk and ensure safe pregnancies. Depending on the severity, management may include: Low-dose aspirin Heparin injections during pregnancy Warfarin for long-term anticoagulation in non-pregnancy conditions Lifestyle modifications such as hydration, avoiding smoking, and mobility on long flights Final Thoughts With proper treatment, individuals with APS can lead completely normal lives. The key is early detection. Awareness can help prevent major blood clotting episodes, improve maternal and foetal outcomes, reduce long-term complications, and provide psychological relief to couples with unexplained miscarriages.
Optimising Maternity Operations & Reducing C-Section Burden Through Evidence-Based Protocols

Optimising Maternity Operations & Reducing C-Section Burden Through Evidence-Based Protocols Optimising Maternity Operations & Reducing C-Section Burden Through Evidence-Based Protocols Reference: Published in Healthcare Radius Magazine, December 2025 — Pages 27–31. High C-section rates have become a major concern, rising globally to 20–21%. In India, they have increased from 21% in 2015–16 to 30–35% today, especially in private hospitals. Major factors responsible include literacy, organisational environment, financial incentives, sociocultural pressures, diet, lifestyle changes, and lack of physical activity. To increase natural birthing rates, women must be guided towards healthy habits right from early pregnancy. Low glycemic index food helps maintain optimal baby weight and reduces maternal health complications like gestational diabetes. Antenatal visits should include education on natural birthing advantages. Obstetricians should actively remove myths and reduce fear about normal labour. Trimester-wise personalised exercises improve strength, flexibility, and safety. Including partners builds emotional connection and confidence. Customized diets—high protein, balanced carbs, essential vitamins, minerals, and adequate fats—are crucial for maternal and fetal health. Simple lifestyle habits like walking, meditation, natural exposure, and pelvic floor strengthening significantly support natural labour. The process of normal labour must be explained to the pregnant woman, her partner, and family during the last trimester (34–36 weeks). This includes understanding true vs. false labour, warning signs, and when to contact the hospital. Loose cord around the neck or previous C-section is not always an indication for surgery. Transparent communication empowers women and supports informed decision-making. Respectful maternity care groups help pregnant women share experiences and build positive attitudes toward natural birth. Shared decision-making, partogram monitoring, continuous fetal heart tracking, and labour analgesia enhance safety and outcomes. A birthing companion helps reduce perception of labour pain by nearly 50%. Active management of labour can reduce delivery time and lower maternal and fetal complications. Encouraging equal compensation for normal delivery motivates hospitals to support natural birthing over unnecessary C-sections. Enhancing Labour Management Through Education, Communication & Clinical Efficiency Normal labour education during 34–36 weeks prevents last-minute panic and improves timely hospital arrival. Active clinical management shortens labour duration and reduces complications for both mother and baby. Hospitals should build a “no-blame” safety culture where staff can report near-misses and incidents without fear. Medical directors must conduct regular morbidity and mortality audits to learn from incidents and refine protocols. Such systems improve transparency, strengthen safety, and reduce litigation risk. How Hospitals Can Improve Outcomes, Reduce Litigation & Strengthen Quality Scores 1. Build a Culture of Safety – Encourage incident reporting without fear. – Conduct regular audits to improve processes. – Strengthen governance and documentation. 2. Standardize Clinical Protocols – Follow evidence-based treatment pathways. – Mandatory protocol-driven decisions for high-risk cases. – Update guidelines regularly as per WHO and national standards. 3. Strengthen Documentation & Communication – Maintain accurate records. – Use structured consent forms. – Train teams in empathetic communication. 4. Empower Patients Through Education – Use shared decision models. – Provide simple educational materials. – Implement strong grievance resolution systems. 5. Continuous Training & Simulation – Conduct emergency drills and simulation training. – Prioritise competency-based evaluations. – Encourage empathy-based learning. 6. Ensure Transparency & Support – Follow open disclosure during complications. – Offer emotional support to patients and families. – Support healthcare workers to avoid burnout. 7. Use Digital Health Tools – Implement EMRs for accurate documentation. – Use decision support alerts for clinical safety. 8. Promote Respectful, Patient-Centred Care – Adopt “Respectful Maternity Care” standards. – Prioritise dignity, privacy, consent, empathy, and compassion. Strengthening safety systems, documentation, and respectful care improves outcomes, reduces litigation risks, and builds true “Care Through Trust.”
Diabetes During Pregnancy: Causes, Risks, and What You Should Do

Diabetes During Pregnancy: Causes, Risks, and What You Should Do Diabetes During Pregnancy: Causes, Risks & What You Should Do Pregnancy is a beautiful time for every woman. During this period, when a baby grows in the womb, there is a special happiness on the mother’s face. However, hormonal changes are also at their peak. Because of these hormonal changes, blood sugar levels sometimes rise and sometimes fall, increasing the risk of diabetes. According to an ICM report, the risk of diabetes among pregnant women in India is significantly higher. If you are pregnant and wondering what to do if diabetes occurs during pregnancy or if your blood sugar fluctuates, Dr. Vinod Bharti explains the correct guidance in this video: Watch the full explanation here. There are two types of diabetes that can occur during pregnancy: Old Diabetes: Diabetes that exists before pregnancy. Gestational Diabetes: Diabetes that develops during pregnancy. If the patient has old diabetes, their treatment continues normally. The most important point is that the HbA1c level should be below 6.5 for at least 3 months before planning pregnancy. This helps ensure normal growth and development of the baby. The treatment for old diabetes continues under a physician, with a switch to safer medication options suitable for pregnancy. Management during pregnancy mainly includes diet, exercise, and medication. For diet management, carbohydrate intake should be reduced but not completely eliminated, as it is essential for the baby’s growth. Protein intake should be increased, and walking for 15–20 minutes after every meal is highly beneficial. Eating every 2–3 hours helps prevent sudden sugar spikes. The main reason diabetes develops during pregnancy is the placental lactogen hormone, which reduces the effectiveness of insulin. This is why even women with no previous history of diabetes can develop gestational diabetes. In India, this affects nearly 10–15% of pregnancies. Walking for 15–20 minutes after every meal naturally helps reduce glucose levels when insulin action decreases. If sugar levels are not controlled through diet and exercise alone, medication is recommended under medical supervision.
Prefer Natural Delivery Over C-Sec? 7 Steps To Prepare For The Same, As Suggested By Gynaecologist

Prefer Natural Delivery Over C-Sec? 7 Steps To Prepare For The Same, As Suggested By Gynaecologist Prefer Natural Delivery Over C-Sec? 7 Steps To Prepare For The Same, As Suggested By Gynaecologist For pregnant women, all the nine months come as a rollercoaster ride. For some, it is deciding whether they should go for a natural delivery or a C-section/cesarean section. Most of them, due to established societal norms, prefer natural birth since that comes with a lot of reported benefits. Whatever you opt for, following a plan is essential. Our expert gives a comprehensive list covering the same. For pregnant women, all the nine months come as a rollercoaster ride. For some, it is deciding whether they should go for a natural delivery or a C-section/cesarean section. Most of them, due to established societal norms, prefer natural birth since that comes with a lot of reported benefits. Whatever you opt for, following a plan is essential. Dr. Vinoad Bharrati, obstetrician and gynaecologist, director, Elite Momz, Unit of Rising Medicare Hospital, gives a comprehensive list covering what to follow if you are pregnant or planning a pregnancy. 7 Steps to Ensure A Smooth Natural Delivery “Planning of giving birth ideally starts with conception. From the initial visit to the antenatal clinic of a pregnant lady, the correct treatment, diet, and exercise, all play very important roles,” says Dr. Bharrati. In the first trimester, ascertaining the correct delivery date is crucial. “Further sonography helps obstetricians detect any deviation from the normal course of pregnancy and any abnormality in babies,” adds the doctor. Thus, for a successful gestation and preparation for a natural delivery, if at all, take note of the following seven steps, recommended by Dr. Bharrati: Attend Antenatal Visits, Conduct Family DiscussionsDuring antenatal visits, clinicians can detect challenges or complications related to pregnancy and treat them timely. At this stage, the couple also discusses further process of birth with their family members, friends, and seniors. After everything, the pregnant lady might be able to decide about the birth plan. Maintain A Diet ChartDiet during pregnancy influences the baby’s development, avoids complications because of deficiencies, and prepares the woman’s body for childbirth. So correct diet choices ultimately will benefit her and the child within the womb. Explaining Childbirth ProcessAs the third trimester begins, doctors should discuss the entire process of childbirth with the couple. They must explain the advantages and disadvantages of natural birthing and Caesarean section. Even though a natural birth plan has many benefits compared to caesarean section, the woman’s medical conditions should determine the correct choice. Childbirth ExercisesChildbirth exercises help a woman cope with the physiological changes of pregnancy and prepare her body for natural birthing, thus contributing to the baby’s natural development. The pregnant lady should start exercises once advised by the treating clinician, that is after the placenta’s location is confirmed and other complications like the risk of preterm birth are ruled out. A few weeks before the due date, do antenatal exercises that widen the pelvis and prepare the birth passage. The partner and family members should participate in these plans to motivate the women. Accompany the WomanThe ideal person to accompany a pregnant woman as she gives birth should be a partner, mother, or midwife. The companion is taught techniques to comfort the lady and this training helps decrease the woman’s pain intensity by about 50% and increases the chance of successful natural birth. Other options for pain relief like entonox and epidural analgesia are also discussed prior to the onset of labour. Educate the WomanThe pregnant woman should be made aware of pelvic examination, artificial rupture of membranes, various steps of normal labour, options of water birth, episiotomy, instrumental delivery options, etc. If the couple is well aware of all things necessary, they can make the right decision. Prepare ChecklistThe checklist of birthing preferences should mention demographic details, clinical details, ambient environment preferences, music preferences, birth companion preferences, non-medicinal pain relief techniques preferences, labour techniques preferences, medications consent, necessary interventions consent, position preferences, after birth umbilical cord cutting preferences, lactational preferences, etc. The same note must be given to the partner, obstetrician, birth companion, and labour ward team.
Postpartum Recovery: Top 8 Effective Tips To Support Physical and Mental Health of New Moms Post-Delivery

Postpartum Recovery: Top 8 Effective Tips To Support Physical and Mental Health of New Moms Post-Delivery Postpartum Recovery: What You Should Do To Support A New Mom? Post-Delivery Care Tips: Starting from the process of ovulation, fertilization, implantation, the appearance of the first heartbeat, the development of the baby, physical changes in pregnancy, emotional changes in pregnancy, and the process of labour, till childbirth, any woman confronts many changes in body and mind. The postpartum period is defined as a period of six weeks from the birth of a child. The early postpartum period is the first week after childbirth. The early postpartum period is very dynamic with changes in both body and also mind as compared to the late postpartum period. The postpartum period involves many risks like postpartum haemorrhage, perineal trauma, Central and venous sinus thrombosis, eclampsia, anaemia etc. It also involves the risk of postpartum depression. In this article, Dr. Vinoad Bharrati, Obstetrician and Gynaecologist, Director, Elite Momz unit of Rising Medicare Hospital, tells us more about how to take care of a new mom’s mental and physical health and deal with postpartum issues. Postpartum Recovery: Top 8 Tips During the early postpartum period, the lady, partner, family members, doctor and team should take care of the diet of the pregnant woman. The diet should include a high-protein diet with plenty of liquids, vitamins, and minerals. Diet pattern usually changes regionwise, it should consist of a balanced diet with plenty of liquids. During the early postpartum period, the recovery of the body is at a faster pace. There are many changes which are taking place such as the adjustment of body fluids in different compartments like intravascular, extravascular and third space. Lady is experiencing more passage of urine, more sweating, and more dehydration during the early postpartum period. Blood volume is shifting from the reproductive system to the circulatory system so there is a possibility of volume overload. Blood pressure may increase in the early postpartum period. Fluid leaks are happening through smaller blood vessels so increase in body swelling, and increased chances of postpartum convulsions. Due to sedentary situations and dehydration, patients may have thromboembolic episodes in the early postpartum period. Due to lack of sleep, the lady always has mental stress. On one side the woman is free from different pregnancy symptoms and on another side, she is facing different changes in her body, and mind with the additional responsibility of taking care of her baby. The whole family along with the husband should be counselled for parenting before the delivery of a child. It will help in effective parenting, good breastfeeding, and family bonding and decrease the chances of postpartum depression. Mother should be pampered and taken care of. During the early postpartum period, establishing breastfeeding at the earliest possible time is very important for the health of mother and baby. For breastfeeding, family support is most important along with breastfeeding education to the mother. Breastfeeding also helps in smoother recovery of just delivered ladies. Many women face problems with back pain during the postpartum period. The usual reason for back pain is the posture of a lady while breastfeeding. Back pain due to spinal anaesthesia is nearly a myth. To deal with this back pain, ladies are advised for exercises which are different from normal delivery as compared to a Cesarean section. Also, the diet should be rich in calcium and supplementation of calcium medications are being provided regularly by their clinicians. Many women are worried about their increased belly size. The size of the uterus becomes normal to the pre-pregnancy size after six weeks from delivery day. So most importantly the tone of abdominal muscles should be corrected with the help of exercises. Advised by professionals. Binding the abdomen is definitely not going to help to reduce the size of the belly. Usually stitches at the wound site of the perineum in case of normal delivery and on the abdomen, in case of Cesarean, usually heal in 8 to 10 days. The tensile strength of these areas will nearly come to 90% of the original in six weeks after delivery. Good hygiene practices are advised along with good nutrition, antibiotics, and a few analgesics for a shorter time. Any kind of fever or medical condition till 6 weeks after delivery is considered a postpartum complication unless and until proven otherwise. So a clean and safe environment is essential at the place of confinement. During the postpartum period every organ is coming back to normal functioning so the ovary does, but it is very irregular in the initial phase. Lactational mothers may have irregular menstruation patterns with irregular ovulation, this increases the chance of unwanted pregnancy. To mitigate this issue, contraception counselling is advised at 6 weeks after delivery for couples. In the postpartum period, there is an opportunity to complete the HPV vaccination to prevent cervical cancer. Immediately after delivery before discharge from the hospital, the lady can receive the first dose of HPV vaccine and later she can complete it during the postpartum period of 6 months. Overall the journey of pregnancy is very happening in different aspects. Similarly, the early postpartum period (initial 1 week) may become more stormy physically, then 1 week to 6 weeks period may bring a few psychological challenges and very late 6 weeks to 6 months is usually less stormy physically and mentally but still exhausting for lactating mothers. So mother and baby require tender and supportive care during the whole postpartum period.
Art of Forceps Delivery: Expert Explains The Techniques, Benefits, Risks, and Considerations
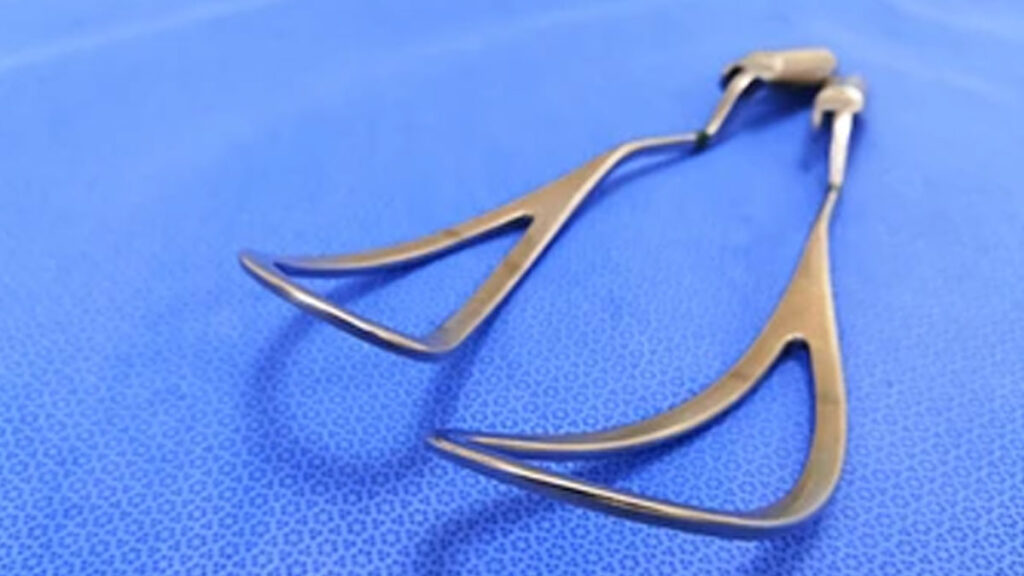
Art of Forceps Delivery: Expert Explains The Techniques, Benefits, Risks, and Considerations Art of Forceps Delivery: Expert Explains The Techniques, Benefits, Risks, and Considerations : Forceps delivery is a technique where forceps are used to gently grasp and guide the baby through the birth canal. Learn about its benefits, risks, procedures, and key considerations for both mother and baby. Click here to read more about forceps delivery. Have you ever wondered what happens when labour doesn’t progress as expected? Or how do doctors manage situations where delivery needs a little extra help? In those moments, forceps delivery can be a lifesaver. While cesarean sections and vacuum deliveries are more commonly discussed, forceps, a technique that has been around for centuries still play a crucial role in assisting women through difficult labour. We spoke to our expert Dr Vinoad Bharrati, Obstetrician and Gynaecologist, Director, Elite Momz, unit of Rising Medicare Hospital, Pune, who guides us through this often-overlooked method, explaining how it works, when it’s needed, and the benefits it offers for both mothers and babies in specific circumstances. Table of Content:- Indications for Forceps Delivery Maternal Indications: Foetal Indications: The Instrument Set Types of Forceps Application Prerequisites for Forceps Delivery Technique For Forceps Delivery When to Abandon the Procedure Advantages of Forceps Delivery Risks Involved The Role of Forceps in Modern Obstetrics “Forceps have a rich history in obstetrics, once considered a royal treasure. In ancient times, many women lost their lives and babies due to obstructed labour. It was caregivers like Chamberlain who recognised the need for forceps and began using them for the greater good of all women. At a time when cesarean sections were risky, forceps delivery became a breakthrough,” said Dr Bharrati. In modern obstetrics, however, the use of forceps has declined significantly, with only about 1% of vaginal deliveries involving forceps. While vacuum deliveries are more common, forceps are still more successful in achieving vaginal delivery. Fear of litigation and lack of training have contributed to this decline, but forceps remain an important tool for shortening the second stage of labour. According to a 2010 study, forceps delivery is a procedure where forceps are inserted into the vagina to gently grasp the baby’s head and assist in guiding it through the birth canal. Forceps may be the preferred method for delivering premature babies due to the higher risk of cephalohematoma and intracranial haemorrhage with vacuum extraction. Additionally, certain medical conditions, such as cardiac, respiratory, and neurological issues, can prevent the necessary maternal effort for successful vacuum extraction during the second stage of labour, as stated in the British Medical Journal (BMJ). Indications for Forceps Delivery Forceps can be used in labour for both maternal and foetal indications: Maternal Indications: Maternal exhaustion Cardiac disease Epilepsy in maternal side-prolonged second stage Foetal Indications: After coming ahead of the breech In preterm as a protective cage Foetal distress with the head descending below the ischial spines The Instrument Set “The forceps instrument set consists of two blades: left and right, designed for maternal side application. The blades include a handle, lock, shank, and fenestrated blade. There are different types of forceps, such as Kielland, Simpson, and Wrigley’s, each with specific curves: cephalic and pelvic,” said Dr Bharrati. Types of Forceps Application The process of using forceps is called a forceps application. Dr Bharrati listed the types of forceps applications as follows: Outlet forceps Low forceps Midcavity forceps High forceps In modern obstetrics, only outlet and low forceps are used and midcavity and high forceps are not used due to the high complication rate. Prerequisites for Forceps Delivery For a forceps-assisted vaginal delivery, the following prerequisites must be met: Informed consent Experienced obstetrician The cervix should be fully dilated Complete empty urinary bladder Foetal head visible at introitus Adequate pelvis Foetal weight estimated before labour Known foetal head position Readiness for a backup plan if the forceps application fails Technique For Forceps Delivery In clinically indicated situations, and when all prerequisites are met, local anaesthesia or epidural anaesthesia is administered. A right mediolateral episiotomy (cut in the perineum) is performed to prevent injury to the anal sphincter. “The forceps application starts by positioning the left blade along the pelvic curve and the right blade along the cephalic curve. If both blades lock properly, it indicates the correct application. If the blades fail to lock, the procedure should be discontinued. Once both blades are securely applied, the obstetrician applies a pull using the forearm in a downward and outward direction. After the foetal head emerges from the perineum, the blades are unlocked and removed, and the delivery proceeds as per routine protocol,” explained Dr Bharrati. When to Abandon the Procedure No descent of the head despite pulling Forceps do not lock properly The foetal head does not emerge after three pulls Advantages of Forceps Delivery Avoidance of Cesarean Section: Forceps delivery helps avoid the need for a cesarean section. Lower Morbidity: Compared to a cesarean, forceps delivery has less morbidity. Immediate Mobility: Women can become mobile right after the procedure. Less Strain on the Heart: Forceps reduce the load on the heart during the second stage of labour. Assisting Exhausted Mothers: It provides relief to mothers who are exhausted or have cardiac/neurological conditions, reducing the duration of the second stage of labour. Cost-Effective: Unlike cesarean sections, forceps delivery does not require expensive instruments or electrical equipment. Risks Involved Maternal perineal injuries Excessive bleeding Foetal injuries The Role of Forceps in Modern Obstetrics “In skilled hands, forceps can be a valuable tool in avoiding cesarean sections, especially in difficult or preterm labour situations. They can also assist in breech deliveries, particularly in the second twin. Failure of forceps is much less as compared to vacuum delivery. The procedure also eliminates the need for maternal effort, offering a safer alternative for exhausted mothers,” said Dr Bharrati. Institutions that use forceps regularly tend to have lower cesarean section rates, highlighting its potential for preserving vaginal deliveries. Furthermore, the use of forceps
Body Bias and Natural Birth: What Plus-Size Pregnant Women Need to Know

Body Bias and Natural Birth: What Plus-Size Pregnant Women Need to Know Body Bias and Natural Birth: What Plus-Size Pregnant Women Need to Know Body bias keeps many plus-size pregnant women from choosing to deliver naturally, but it doesn’t have to, says Obstetrician. With the right doctor, the right preparation, and a hospital that knows what it’s doing, plenty of plus-size women have healthy, uncomplicated births. Pregnancy is supposed to be this magical, life-changing journey, but for plus-size women, it often comes with an extra layer of anxiety—especially around the idea of a natural delivery. Somewhere along the way, many women started believing that a higher BMI automatically means a C-section. Doctors won’t even try for a normal delivery, right? Well, that’s actually not true. Being overweight or obese doesn’t close the door on a natural birth. Obesity in pregnancy usually means a BMI of 30 or more, and yes, it brings some risks. But health isn’t a one-size-fits-all formula. A woman’s age, whether she has had babies before, her general health, and even how the baby is growing inside—all of these factors come together to shape her birth experience. The real takeaway is simple: weight is only one chapter in a much bigger story. Good obstetric teams deal with these situations all the time. With early and proactive care, most risks can be managed without drama. For more perspectives on pregnancy health and delivery decisions, you can also explore articles like this one from ETV Bharat: Read full article. Dr. Vinoad Bharrati, Senior Consultant Gynaecologist and Obstetrician, Founder and Director, Elite Momz – Rising Medicare Hospital, Pune, says, “Many women with obesity go on to have smooth vaginal births. The chances go up when the pregnancy is monitored right from the start, weight gain stays within healthy limits, blood pressure and sugar levels are under control, and labour is handled with mobility, pain relief, and continuous monitoring. A hospital that has strong obstetric, anaesthesia, and neonatal support makes all the difference when it matters most.” Possible Complications Of course, the journey isn’t without its bumps. Obesity can increase the chances of: Gestational diabetes mellitus (GDM) High blood pressure or gestational hypertension Big babies (macrosomia) Longer or slower labour process Higher need for induction of labour However, these challenges do not necessarily require surgical delivery. Properly managed, many plus-size women avoid complications and progress normally through labour. Tips for Moms-To-Be There are some simple but powerful steps that can improve the chances of natural childbirth. Gynaecologist and Obstetrician Dr. Bharrati suggests: Starting antenatal care early helps catch issues like anemia or high sugar before they become problems. Keeping weight gain under control: 7–11 kilos for overweight women and 5–9 kilos for women with obesity. A good nutritionist can make this easier. Staying physically active—walking, prenatal yoga, pelvic exercises, or even swimming (if advised)—builds stamina and supports natural labour. Fetal medicine helps monitor the baby’s growth accurately. Regular scans and Doppler studies show whether the baby is growing too fast, too slow, or just right, so everyone can prepare well. When labour begins, small changes make a big difference for plus-size women, such as upright positions, freedom to move, good pain relief like epidurals, and strong midwifery or nursing support. These help the pelvis open naturally and support the rhythm of labour. Sometimes, a C-section might be advised if: Blood pressure shoots up Diabetes is poorly controlled Baby’s size is significantly large Poor labour progress on partogram despite interventions Fetal heart monitoring shows distress Even in these situations, the decision is based on medical safety, not BMI alone. At the end of the day, obesity doesn’t decide how your birth story ends. With compassionate doctors, evidence-based guidance, and a hospital that respects your choices, many plus-size women go on to have healthy, empowering natural births. The focus should always be on the mother—her body, her pregnancy, her journey—not on assumptions based on weight.
NICU Success Story: A Remarkable Recovery From Severe Respiratory Distres
Hindustan Times Spotlights Dr. Vinod Bharti on Monsoon Gynaecological Care We are proud to share that Dr. Vinoad Bharrati, Director and Consultant Gynaecologist at Rising Medicare Hospital & Elite Momz, Pune, has been featured in Hindustan Times Lifestyle for his expert contribution to women’s monsoon health. I am honored to be featured in Hindustan Times, in an article published on 5th August 2025, where I shared my guidance on the five common gynaecological infections that tend to increase during the monsoon season. In this feature, I discussed how humid weather makes women more prone to fungal, bacterial, and urinary tract infections, the early warning signs they should never ignore, and the essential preventive measures every woman must follow to stay healthy and protected during the rainy season. Here are the key insights I provided: The monsoon’s humidity creates an environment where fungal, bacterial, and urinary tract infections become more common. Women should watch out for early symptoms such as curdy white or foul-smelling discharge, excessive itching, or burning sensation during urination. Lower abdominal pain or discomfort may also indicate a developing infection. I encourage women to adopt preventive habits like wearing cotton innerwear, changing clothes when wet, and choosing loose, breathable garments. Maintaining intimate hygiene is crucial—avoid perfumed soaps or sprays in sensitive areas and always clean public toilet surfaces before use. If any symptoms persist, immediate medical consultation is essential to prevent complications.
Severe Pollution, AQI Levels Highly Dangerous For Pregnant Women, Fetus; Expert-backed Ways To Protect Yourself

Severe Pollution, AQI Levels Highly Dangerous For Pregnant Women, Fetus; Expert-backed Ways To Protect Yourself Severe Pollution: AQI Levels Highly Dangerous for Pregnant Women and Their Babies — Expert-Backed Ways to Protect Yourself Source: Times Now Health Report The air quality across Delhi-NCR has reached hazardous levels, with AQI readings soaring between 350–400, turning the region into a virtual gas chamber. While toxic air impacts everyone, pregnant women and their developing fetuses are among the most vulnerable, with risks ranging from preterm birth to stillbirth. Doctors are urging expectant mothers to take extra precautions, especially during peak pollution hours. Here’s what you need to know—and how you can protect yourself and your baby. Why Air Pollution Is Extremely Dangerous During Pregnancy According to experts, the recent spike in air pollution is life-threatening for both pregnant women and fetuses. Studies show that prolonged exposure to high AQI levels can lead to: Preterm birth (before 36 weeks) Low birth weight Stillbirth Spontaneous abortion Pregnancy-induced hypertension Placental complications “During pregnancy, several physiological changes occur, such as increased tidal volume, lung capacity, and cardiac output. These make pregnant women especially vulnerable to the harmful effects of pollutants—and the fetus becomes equally at risk,” explains Dr. Vinoad Bharrati, Obstetrician and Gynaecologist, Director of Elite Momz at Rising Medicare Hospital, in an interview with Times Now. Dr. Bharrati highlights that pollution has the strongest impact during the first and third trimesters, contributing to complications like preterm birth, postpartum depression, IUGR (Intrauterine Growth Restriction), and uteroplacental insufficiency. How Air Pollution Affects the Mother and Fetus More than 99% of people in urban Indian regions breathe air that fails to meet WHO safety norms. The key culprits are particulate matter (PM2.5 and PM10) produced from fossil fuel combustion, industrial emissions, and vehicular pollution. What Happens Inside the Body? PM10 particles (10 µm) enter the lungs through the respiratory tract and cause inflammation. PM2.5 particles (2.5 µm or smaller) penetrate deeper, traveling from the lungs into the bloodstream. These pollutants can then: Cross the placenta, directly affecting the baby Damage the placenta’s functioning Raise the mother’s blood pressure Trigger asthma attacks and worsen respiratory conditions “When these finer particles enter the bloodstream, they begin producing harmful effects systemically,” Dr. Bharrati adds. Precautions Pregnant Women Must Take During High Pollution Days While completely avoiding pollution is impossible, pregnant women can significantly reduce its impact by following simple, expert-recommended steps: Avoid Going Outdoors When AQI Is High Even with a mask, toxic gases and microscopic particles can be inhaled or absorbed through the skin. If you have asthma, allergies, or respiratory issues—limit outdoor activities as much as possible. Stay Hydrated Drinking plenty of water helps your body flush out toxins and supports optimal organ function. Wear a High-Quality Mask If stepping outside is necessary, wear an N95 or N99 mask for maximum protection. Use an Air Purifier at Home Invest in a reliable air purifier to reduce indoor pollution levels. Indoor plants like snake plants can also help improve air quality naturally. Maintain a Healthy Lifestyle Eat antioxidant-rich foods Rest adequately Avoid strenuous outdoor exercise Keep windows closed during peak pollution hours Final Thoughts Severely polluted air is not just an environmental issue—it is a maternal health emergency. For pregnant women, even short-term exposure can have long-term consequences for both mother and baby. It’s essential to: Stay informed Take preventive measures Follow medical advice Prioritize maternal and fetal health If pollution levels continue to escalate, consult your healthcare provider for personalized recommendations and regular monitoring.
Vaginal Birth After Caesarean Section (VBAC): Is It a Safe Option for Mothers?
Vaginal Birth After Caesarean Section (VBAC): Is It a Safe Option for Mothers? I am honored to share expert guidance in this feature published on October 28, 2024, where I discussed the rising rate of C-sections in India, the safety of choosing a VBAC, and the crucial guidelines mothers must follow to ensure a safe trial of labour after cesarean (TOLAC). The article highlights WHO recommendations, national C-section statistics, and expert-backed advice on when a VBAC can be a safe and successful option. Here are the key insights I provided: According to WHO, C-section rates ideally should not exceed 10%, but globally rates have reached 20–21%. In India, C-section rates have risen from 21% (2015–16) to beyond 30% in recent years. Multiple factors contribute to the rising C-section rate, including literacy, hospital systems, financial incentives, sociocultural reasons, and medical implications. TOLAC (Trial of Labour After Caesarean) should be offered as an option for eligible women. VBAC is the successful vaginal birth outcome of TOLAC, while CBAC refers to cesarean delivery after a failed TOLAC. The success rate of TOLAC is approximately 52–70%, while the risk of scar rupture is only 0.4–1% — significantly lower than commonly feared. VBAC is safe when conducted under strict protocols, with expert obstetricians, full-time availability of anesthesiologists, and immediate access to a well-equipped operation theatre. A detailed history of the previous C-section — including the indication for surgery — must be evaluated before offering TOLAC. The current pregnancy must be free of complications, and the onset of labour must be spontaneous for the mother to qualify. Mothers should be thoroughly counselled on the benefits, process, and risks of TOLAC, including the rare but possible complication of scar rupture. Continuous fetal monitoring, mother’s vital monitoring, the use of partogram, and immediate response to fetal bradycardia are essential for safe TOLAC. The success rate of TOLAC improves significantly with expert hands, proper hospital setup, and correct patient selection. Process of TOLAC: The pregnancy follows a routine course similar to any other pregnancy. The key difference is the selection of a skilled obstetric team and a hospital equipped for emergency intervention. Labour must begin spontaneously; induction is generally avoided. Continuous CTG (cardiotocography) and maternal monitoring is mandatory. Fetal bradycardia is often the earliest sign of scar rupture and requires immediate action. Epidural analgesia may be safely offered for labour pain relief. Benefits of Successful TOLAC (VBAC): Shorter hospital stay Lower maternal morbidity Lower financial burden Fewer abdominal complications Reduced risk of transient tachypnea (TTN) in newborns Risks Involved: VBAC: Maternal and fetal risks are very low. CBAC: Risks are similar to a planned elective C-section. Scar rupture (0.3–1%): Though frightening, this risk is extremely low and can be further minimized by expert monitoring and timely surgical intervention. With expert medical teams, strict monitoring, and clear protocols, TOLAC is a safe and beneficial choice for many pregnant women. Increasing the acceptance of TOLAC can significantly reduce unnecessary C-sections and lower the financial and medical burden for mothers across the country. In the current scenario, financial structures in private hospitals often incentivize C-sections over normal deliveries. If insurance and compensation frameworks begin valuing TOLAC and VBAC equally, more hospitals and obstetricians will be motivated to implement safe VBAC protocols — ultimately improving national childbirth outcomes.
